In 2012, OIG determined that the VHA had mismanaged its Medical Care Collections Fund (MCCF) program. They write:
VHA is authorized to bill third-party health insurance for covered health care provided to veterans at VA and non-VA medical facilities. The MCCF program recovers costs of medical care that VA provides to patients who have coverage under a private health insurance policy. A veteran may have coverage under a personal or spouse’s insurance policy. VA considers a
veteran’s health care billable if the treatment is non-service-connected and the third-party health insurance policy covers the treatment.
This revenue is not a trivial amount of money when collected. VHA reported MCCF third-party insurance collections for FY 2010 was 1.9 billion and for FY 2011, 1.8 billion. I almost hate to link to this study because it’s so frustrating. The VHA needs these funds to provide state-of-the-art care, hire and retain the brightest physicians, and keep the ERs running smoothly 24/7. Other VHA medical budget priorities include traumatic brain injury care, spinal cord injury care, prosthetics , mental health, telehealth, and more.
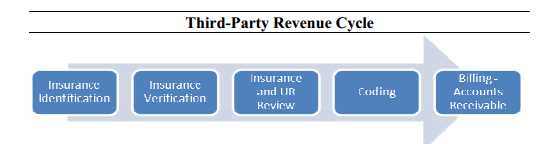
When we see private providers, they follow this basic process, the same one the VHA is supposed to follow:
If administrators can plan Orlando parties (conventions) why can’t get their act together and obtain private insurance information, apply proper coding and bill Aetna, Humana and other private insurance carriers? (The VHA cannot generally bill Medicare but it can bill Medigap Supplemental plans.) The bad news from this audit:
The OIG audited eight sites and found The 8 facilities had almost
2 million unbilled patient encounters on the FY 2010 RNB report which totaled nearly $1.7 billion in unbilled medical services. The majority of this unbilled amount on the RNB report was attributable to a small number of high-value patient encounters.
High-value claims are over $400,000, medium-value claims are $5,000 to $400,000, and low-value claims are less than $5,000. Can you imagine any regional hospital not billing Blue Cross for care worth $300,000 +/-? But back at the VHA ranch, medical committees find time and energy to deny disabled veterans structural alterations, and deny care through their fiscal and ethical mismanagement. And then there is the little matter of co-pays and co-insurance which veterans in some priority groups must pay for VA care and prescriptions. According to the SRC report (page two):
The VA has the authority to bill most health care insurers for nonservice-connected care; any insurer’s payment received by the VA is used to offset ‘‘dollar for dollar’’ a veteran’s VA copayment responsibility.
If the VHA isn’t billing a veteran’s insurance company, then he’s getting screwed out of this dollar-for-dollar offset. (Anyone ever had a co-pay offset by the VA?)
Well, gee, aren’t Priority 8 veterans rich? Living high on the hog? Why can’t they pay $50 a pop to see a VA specialist? And med co-pays? The answer is below.
Why doesn’t our veteran (if under 65) just buy a marketplace private plan? Well, it might be too expensive and Congress won’t allow our veteran to be enrolled in VA care AND buy a ACA plan. Why? Who knows. That would make too much fiscal sense so let’s discriminate against our veterans instead. If you want to buy a ACA plan for the family (that we could then bill), you can’t take advantage of your earned VA health benefit. Oh, and Thank You for your service!![]()



Anything that makes sense to us is lost in translation over at the VA. Very informative piece. Thank you